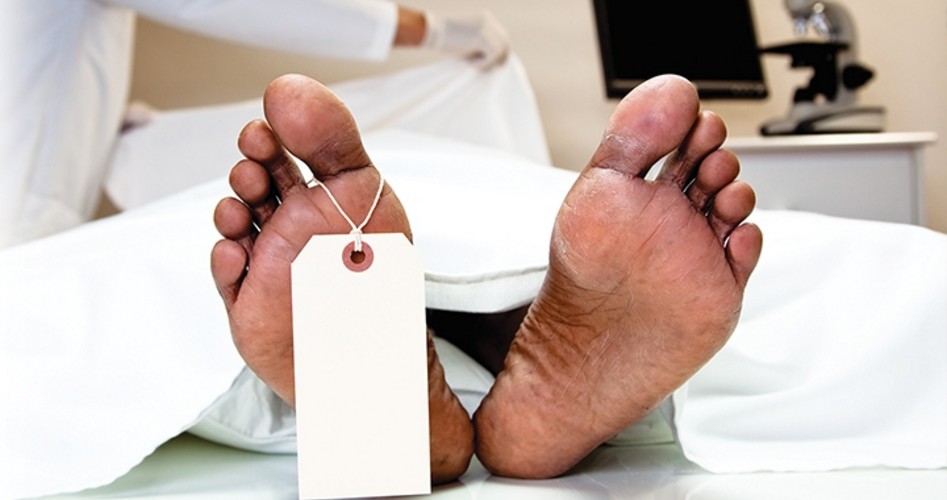
Going With “Fair” Healthcare
Socialized medicine is often touted as our country’s healthcare solution. But it results in market distortions that lead to shortages, delays, and disrespect for life itself.
It was a tragedy that should not have happened. A young woman, just beginning her studies at college where she was pursuing undergraduate work in music and sound production, was found dead in her room roughly a day after she complained of feeling ill.
Twenty-year-old Victoria Hills was, by all accounts, a wonderful young lady who was known for the kindness she showed to others, for her love of walking her dogs on the beach, and for her zest for life.
“Victoria was so full of life,” her mother recalled of her daughter. “She had been in her church choir for 11 years and always played in school concerts. Music was everything to her.”
JBS Member or ShopJBS.org Customer?
Sign in with your ShopJBS.org account username and password or use that login to subscribe.
 Subscribe Now
Subscribe Now
- 24 Issues Per Year
- Digital Edition Access
- Exclusive Subscriber Content
- Audio provided for all articles
- Unlimited access to past issues
- Cancel anytime.
- Renews automatically
 Subscribe Now
Subscribe Now
- 24 Issues Per Year
- Print edition delivery (USA)
*Available Outside USA - Digital Edition Access
- Exclusive Subscriber Content
- Audio provided for all articles
- Unlimited access to past issues
- Cancel anytime.
- Renews automatically