Rx for Healthcare
The Primal Prescription: Surviving the “Sick Care” Sinkhole, by Doug McGuff, M.D., and Robert Murphy, Ph.D., Malibu, California: Primal Blueprint Publishing, 2015, 362 pages, hardcover.
The U.S. healthcare system is sick, largely as a result of myriad government interventions. Nevertheless, there are things individuals can do to stay healthy and avoid the worst aspects of the system. Those are the twin messages of The Primal Prescription: Surviving the “Sick Care” Sinkhole.
The book’s authors are Doug McGuff, an emergency physician and personal trainer, and Robert Murphy, a free-market economist. Combining their expertise yields a volume that not only explains how the healthcare system got so screwed up but offers real-world examples of just how bad things really are — and what to do about them.
JBS Member or ShopJBS.org Customer?
Sign in with your ShopJBS.org account username and password or use that login to subscribe.
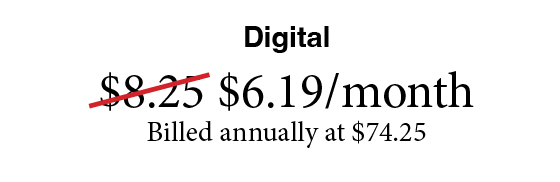 Subscribe Now
Subscribe Now
- 24 Issues Per Year
- Digital Edition Access
- Exclusive Subscriber Content
- Audio provided for all articles
- Unlimited access to past issues
- Cancel anytime.
- Renews automatically
 Subscribe Now
Subscribe Now
- 24 Issues Per Year
- Print edition delivery (USA)
*Available Outside USA - Digital Edition Access
- Exclusive Subscriber Content
- Audio provided for all articles
- Unlimited access to past issues
- Cancel anytime.
- Renews automatically


